- Home
- Common Knee Conditions
- Chondromalacia Patella
Chondromalacia Patella
Written By: Chloe Wilson, BSc(Hons) Physiotherapy
Reviewed by: KPE Medical Review Board
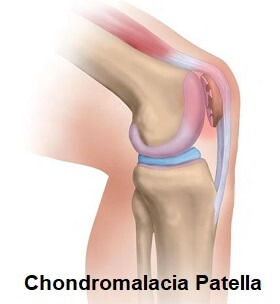
Chondromalacia patella is a common knee condition where there is softening and damage to the cartilage on the back of the patella (kneecap).
Chondromalacia causes front knee pain, swelling and clicking/grinding noises when moving the knee.
It tends to affect young, healthy and often sporty people, most commonly affecting adolescents and young adults. Chondromalacia is more common in women than men.
Chondromalacia patella is frequently misdiagnosed as Runners Knee, which is actually a problem with how the kneecap moves rather than the cartilage itself.
Here we will look at the most common causes and symptoms of chondromalacia as well as the best ways to treat it and the recovery process.
Patella Anatomy
To fully understand what is going on with chondromalacia patella, it helps to understand a little bit about the structure and function of the kneecap. The patella is a small, triangular shaped bone that sits inside the quads muscles at the front of the thigh.
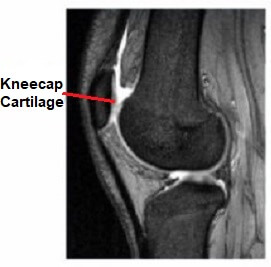
It rests in a special dip know as the patella groove on the front of the thigh bone, the femur, where it moves up and down as you move your leg.
The patella is lined with the thickest cartilage in the whole body which:
- Ensures the patella glides smoothly over the knee bones
- Works as a shock absorber
Not only does the patella help to protect the knee joint, it also helps the quads muscles work more effectively, by reducing the amount of force needed to move the knee.
What Causes Chondromalacia Patella?
Chondromalacia patella is caused by a problem with how the knee cap moves. Instead of gliding smoothly up and down in the patella groove, it shifts over slightly, rubbing against the edge of the groove, causing friction. This causes small tears in the cartilage which get inflamed and cause pain.
Common causes of chondromalacia patella are:
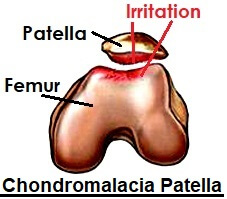
- Muscle Imbalance: In chondromalacia patella, a combination of muscle tightness on the outer knee and muscle weakness on the inner knee affects the position of the kneecap in the patella groove.
This pulls the kneecap slightly to the side so it rubs on the edge of the patella groove, resulting in a lot of friction which ends up damaging the cartilage. This is also known as patella maltracking. - Poor Alignment of the Kneecap: For some people, their patella doesn’t sit in the right position, but rests either too high or too low. Some people are born this way, but it doesn’t become apparent until adolescence.
- Overuse of the Leg: Any activities that place strong, repetitive forces through the kneecaps, e.g. running, jumping, twisting, can damage the back of the cartilage leading to chondromalacia.
- Flat Feet: Having flat feet is another common cause of chondromalacia patella. When the foot arches drop, as with flat feet, it changes the way the forces are distributed through the knee as we walk and run which makes the cartilage more prone to damage.
Chondromalacia Patellae Symptoms
The most common symptoms associated with Chondromalacia Patella are:
- Front Knee Pain: tends to be achy rather than sharp
- Grinding/Grating Sensation: when moving the leg, known as crepitus
- Minor Swelling: usually around the patella
- Tenderness: with any pressure through the kneecap
- Pain On Stairs: tends to worse going downstairs rather than upstairs
- Pain After Prolonged Rest: when you first get up after sitting down for a while
How is Chondromalacia Diagnosed?
Your doctor will normally diagnose patella chondromalacia from your description of symptoms and by carrying out some simple tests.
These may include looking at the movement of the knee, and putting pressure through the knee cap
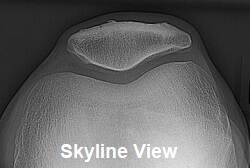
Standard x-rays don’t usually show up the problem, although a “skyline view x-ray” taken from the side of the leg can be used to see the back of the kneecap.
MRI scans are occasionally used to confirm the diagnosis.
Treatment For Chondromalacia
There are a number of different chondromalacia patella treatment options which typically include:
#CommissionsEarned from Amazon on qualifying purchases
1. Knee Straps

Knee straps are a must with chondromalacia patella for anyone who plays sport. They might not look like much but wearing a strap directly under the kneecap really helps take pressure off the joint, which can dramatically reduce knee pain.
Knee straps are simple to use and extremely effective, whatever stage of the rehab process you are at. There are a few different styles, some of which work better than others. LEARN MORE >
2. Knee Exercises
Strengthening and stretching exercises are a vital part of chondromalacia patella treatment. They help to combat any muscle imbalance and improve how the kneecap moves, which takes the pressure off the kneecap. I have never known anyone with chondromalacia patella who has not had muscle imbalance and therefore benefited from exercises. LEARN MORE >
3. P.R.I.C.E
PRICE (Protect, Rest, Ice, Compress, Elevate) is one of the simplest and underused treatments for chondromalacia. When done properly it helps reduce pain and swelling and can speed up recovery. LEARN MORE >
4. Applying Ice
Using ice regularly and before and after activity can help reduce swelling and pain associated with chondromalacia. Not only does this reduce the symptoms of chondromalacia patella, it also helps to speed up the recovery process. LEARN MORE >
5. Shoe Inserts
If are suffering from chondromalacia and you have flat feet, then wearing insoles, known as orthotics, can really help. They simply slip into your shoe and help to correct alignment by supporting the foot arches which helps to reduce the force through the kneecap.
If you are going to use shoe inserts, make sure you wear them in both shoes otherwise you end up with one leg slightly longer than the other which can lead to back and hip problems. You should also start by only wearing them for short periods and gradually build up to allow your body to adjust.
6. Medication
Non-steroidal anti-inflammatories (NSAID’s) such as ibuprofen/Advil will help to relieve the inflammation and pain associated with chondromalacia patella. Always check with your doctor before taking any medication.
7. Taping
Taping can help to realign the patella and take the pressure off the kneecap - particularly useful for sports. Initially, I would recommend a physical therapist applies the tape initially, but once they have found the best taping technique for you, they can teach you how to do it yourself.
8. Modify your Activities
An important part of Chondromalacia Patella treatment is to try and avoid the activities that place pressure through the kneecap.
Limit running and instead try swimming or cycling. If you want to run, ensure you are wearing good shoes with cushioned shoes, and stay off hard surfaces e.g. concrete.
9. Use Knee Pads
Gel Knee Pads are an excellent way to reduce kneecap pain and irritation when you are kneeling. They take the pressure off the back of the kneecap and provide cushioning. There are loads of different options out there, some more effective than others. LEARN MORE >
10. Knee Surgery
Surgery for chondromalacia patella is only considered if nothing else works and the pain is really affecting your daily life.
Most commonly it will be a knee arthroscopy, keyhole surgery where they make 2-3 small holes around the knee and insert a camera. The surgeon cuts any tight ligaments to allow the patella to sit in the right place in the groove and/or shave off any damaged bits of cartilage so the kneecap can move correctly.
Recovery Process
Chondromalacia Patellae usually settles down with medication and exercises but it is likely to take a few months.
The sooner you get going with exercises, the sooner it will get better. Check out the strengthening exercises and stretches sections for exercises you can do at home to help. Surgery is rarely necessary.
Common Misdiagnosis
Front knee pain is commonly misdiagnosed as chondromalacia patellae when it isn’t. Another common cause of similar pain is Runners Knee aka Anterior Knee Pain or Patellofemoral Pain.
While the symptoms can
be similar, there is not the softening and damage to the cartilage that
is characteristic of chondromalacia. Treatment is however
similar for both conditions.
If chondromalacia patella doesn't sound quite like your problem, visit the knee pain diagnosis section for help working out what your problem is and what you can do about it.
You may also be interested in the following articles:
- Inner Knee Pain
- Outer Knee Pain
- Swelling Below The Knee
- Burning Knee Pain
- Knee Pain At Night
- How To Do Stairs With Knee Pain
- Knee Pain Diagnosis
Page Last Updated: 19/02/24
Next Review Due: 19/02/26