- Home
- Common Knee Conditions
- Bursitis
- Infrapatellar Bursitis
Infrapatellar Bursitis
Written By: Chloe Wilson, BSc(Hons) Physiotherapy
Reviewed by: KPE Medical Review Board
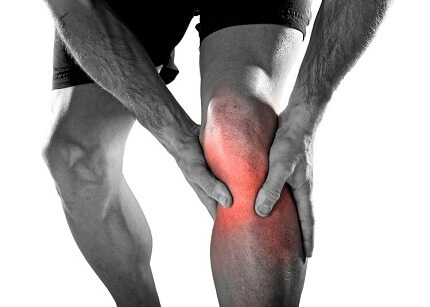
Infrapatellar bursitis causes pain and swelling at the front of the knee, just below the kneecap.
Also known as Clergyman’s Knee, infrapatellar bursitis develops when there is irritation and inflammation of one of the small fluid-filled sacs in the knee.
This may be from overuse, spending lots of time on your knees, an injury or underlying knee condition.
With proper treatment, most cases of infrapatellar bursitis will settle within a few weeks. Clergyman's knee is the most common cause of swelling below the knee.
Here we look at the common causes, symptoms, diagnosis and treatment of infrapatellar bursitis as well as how long it takes to recover.
What Is Infrapatellar Bursitis?
Infrapatellar bursitis affects one of the knee bursa. Bursa are small fluid-filled pockets or sacs filled that sit between bones, muscles and tendons. They provide cushioning and lubrication, allowing the soft tissues to slide smoothly over each other or over bone without any friction.
There are a number of different bursa around the knee. The infrapatellar bursa is found just below the kneecap and sits around the patellar tendon, the large tendon that connects the quadriceps muscles to the lower leg.
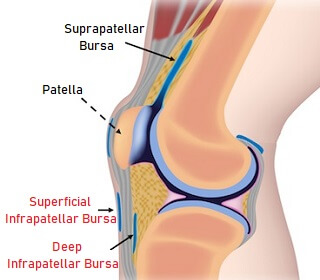
The infrapatellar bursa is actually made up of two sacs:
Superficial Infrapatellar Bursa: sits in front of the patellar tendon, between the tendon and the overlying skin
Deep Infrapatellar Bursa: Sits underneath the patellar tendon, between the tendon and the shin bone (tibia)
For all intents and purposes, the superficial and deep infrapatellar bursae are treated as one bursa.
The infrapatellar bursa protects the patellar tendon as you bend and straighten the knee, allowing it to glide smoothly and freely over the tibia as you move.
Repetitive irritation, pressure or friction on the bursa can cause it to produce excess fluid. This is a natural protective mechanism to prevent damage to the knee, but as the fluid builds up, the bursa starts to swell, resulting in bursitis. If left untreated, the fluid may thicken and harden. In extreme situations, calcification may appear in the bursa.
Common Causes Of Infrapatellar Bursitis
Common causes of infrapatellar bursitis include:
- Frequent Kneeling or Crawling: when you are on your knees, excess pressure goes through the infrapatellar bursa, squashing it. This repetitive pressure causes the bursa to gradually thicken and swell
- Overuse: Activities that require frequent bending of the knee, such as running, jumping, kicking, climbing or stairs, places a lot of friction on the bursa causing it to swell, resulting in infrapatellar bursitis
- Injury: A sudden, hard blow to the front of the knee can damage the infrapatellar bursa directly. Knee injuries can also cause bleeding and excess fluid to build-up around the knee which seeps into the infrapatellar bursa, causing it to swell
- Knee Conditions: Infrapatellar bursitis often develops secondary to other knee problems, most commonly jumpers knee (patellar tendonitis) and Osgood Schlatters Disease
- Infection: Septic bursitis develops when bacteria enter the infrapatellar bursa through a cut in the skin, causing an infection
Infrapatellar Bursitis Symptoms
Infrapatellar bursitis symptoms usually come on gradually over a few weeks or months and consist of:
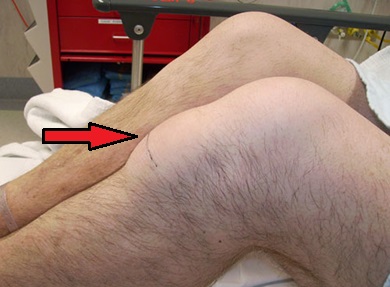
- Swelling: There is often swelling at the front of the knee with infrapatellar bursitis. There may be a squashy pocket of fluid at the front of the shin, just below the kneecap which is usually tender to touch
- Knee Pain: Pain from infrapatellar bursitis is usually felt at the front of the knee, just below the kneecap, causing pain just below the knee. It may extend down the front of the shin too. Infrapatellar bursitis pain typically gets worse when bending the knee and climbing stairs. Kneeling is usually very painful as it squashes the inflamed bursa
- Redness & Warmth: There may be an area of redness at the front of the knee, particularly with septic infrapatellar bursitis, and the skin may feel warm to touch
- Difficulty Sleeping: Sleep is often affected with bursitis with frequent waking due to pain surges when bending the knee or rolling over as you sleep
- Knee Stiffness & Weakness: The pain from clergyman’s knee may cause you to use the knee less which in time can lead to stiffness and weakness in the joint
Diagnosing Clergyman’s Knee
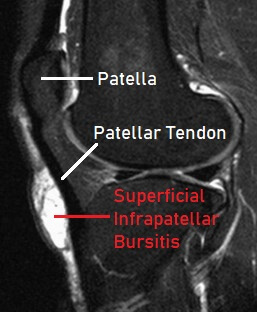
To diagnose infrapatellar bursitis your doctor will start by asking you about your symptoms, such as how the pain started and what aggravates it. They will then examine your knee and perform various tests to look at the integrity of the different knee structures.
They may send you for an x-ray to rule out an underlying bone spur or bony injury. If they suspect soft tissue damage then they will send you for an MRI scan.
If they suspect septic bursitis, your doctor will remove some fluid from the bursa with a needle and have it tested for infection.
Differential Diagnosis
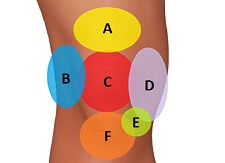
There are a number of other conditions that cause front knee pain and pain below the knee with similar symptoms to infrapatellar bursitis. If there is minimal or no swelling at the front of the knee, it might be that something else is going on such as:
- Jumpers Knee: inflammation in the patellar tendon itself
- Osgood Schlatters: Damage to the bone at the insertion of the patellar tendon. Common in children following a growth spurt
- Prepatellar Bursitis: Inflammation of the bursa directly in front of the kneecap
- Runners Knee: A problem with how the kneecap moves
- Chondromalacia Patella: Damage to the cartilage that lines the back of the kneecap
- Plica Syndrome: Inflammation of the lining of the knee joint
#CommissionsEarned from Amazon on qualifying purchases
How Is Infrapatellar Bursitis Treated?
There are a number of treatment options for infrapatellar bursitis including:
- Rest: Avoid activities and exercises that aggravate your knee as the bursa needs time to heal. If you don’t rest, the infrapatellar bursa will keep getting irritated and inflamed and will take longer to heal
- Keep Pressure Off: Keep as much pressure off your knee as possible – try to avoid kneeling or crawling altogether. If you have to kneel, either wear knee pads or kneel on a cushion. And it can really help to make some simple changes to how you go up and down stairs, particularly if that is something which hurts LEARN MORE >
- Ice: Regularly applying ice to the front of the knee is a great way to reduce the pain and inflammation from infrapatellar bursitis, but it is important to follow the recommended guidelines – visit the knee ice treatment section to find out more
- Medication: Your doctor may advise taking non-steroidal anti-inflammatories (NSAID’s) e.g. ibuprofen/Advil to help reduce pain and swelling with bursitis
- Aspiration: Your doctor can remove excess fluid from the infrapatellar bursa using a needle and syringe. They may inject corticosteroids into the bursa at the same time to further reduce pain and swelling
- Physical Therapy: Strengthening exercises and stretches are an important part of rehab with infrapatellar bursitis to regain full strength, mobility and function in the knee. Muscle weakness and tightness often places increased pressure on the bursa so exercises are really important to make sure the condition doesn't return in the future
- Surgery: If symptoms persist despite treatment for infrapatellar bursitis, then your doctor may suggest surgery to remove the bursa completely, however this is only usually done as a last resort
One of the big aims with infrapatellar bursitis treatment is to reduce the fluid in the bursa which can leak out into the knee. There are lots of different options that can help - find out more in the swollen knee treatment section.
How Long Does Bursitis Last?
Infrapatellar bursitis can last for anything from a couple of weeks to a few months. If you follow the recommended treatment above, particularly resting from aggravating activities, then symptoms of clergyman’s knee should settle within a few weeks. Generally, the sooner you start treatment, the quicker you will recover.
If infrapatellar bursitis has developed secondary to other knee problems, such as patellar tendon inflammation (Jumpers Knee) or Osgood Schlatters Disease, then it may take 3-6 months for things to fully settle down. It is really important to treat the underlying cause of infrapatellar bursitis, not just the swelling, otherwise the condition is likely to return.
Infrapatellar Bursitis Summary
Infrapatellar bursitis is the most common cause of pain and swelling below the kneecap.
Repetitive friction or pressure results in excess fluid collecting in the bursa, leading to infrapatellar bursitis.
Frequent kneeling is a common cause of infrapatellar bursitis, hence the name Clergyman's Knee.
The infrapatellar bursa is actually two bursa, the superficial infrapatellar bursa, found in front of the patellar tendon, and the deep infrapatellar bursa, found underneath the patellar tendon.
Infrapatellar bursitis treatment starts with resting from all aggravating activities and may include medications, exercises, physical therapy, steroid injections, aspiration and occasionally surgery.
You may also be interested in the following articles:
- Front Knee Pain
- Pain Below The Knee
- Knee Swelling
- Knee Bursitis
- Knee Pain Kneeling
- Knee Pain Diagnosis Chart
Related Articles
References
1. Radiopaedia - Infrapatellar Bursitis. By Dr A. Al Kabbani and Dr M. Morgan et al
2. Study.com - Deep & Superficial Infrapatellar Bursitis: Symptoms & Treatment. By Dr A. Monroe
3. BMJ Best Practice - Bursitis. By Dr N. Maffulli, Dr U. Longo, Dr V Denaro et al. August 2019
Page Last Updated: 06/06/24
Next Review Due: 06/06/26