- Home
- Common Knee Conditions
- Bone Spurs Knee
Bone Spurs In Knee
Written By: Chloe Wilson, BSc(Hons) Physiotherapy
Reviewed by: KPE Medical Review Board
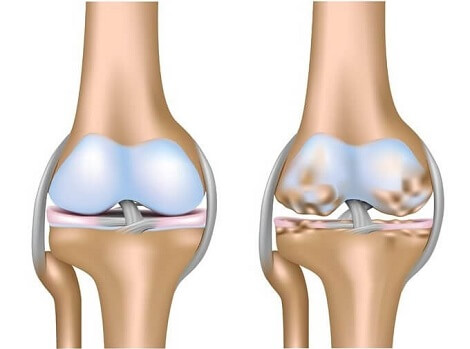
Bone spurs in the knee are a common problem, particularly in people over the age of 60.
In some cases, knee bone spurs cause no symptoms at all, but for other people, they may result in both pain and stiffness and can really affect daily life.
Bone spurs are hard, bony lumps that grow on the surface of joints through a process called osteophytosis, forming bumps or ridges. In some cases, bone spurs cause no symptoms at all, but if they start to rub against other bones or soft tissues, they may result in both pain and stiffness and can really affect daily life.
Bone spurs on the knee are usually caused by cartilage damage, arthritis and excess pressure through the joint.
Here we will look at what bone spurs in the knee are, how they form, the common causes and symptoms, how they are diagnosed and the best treatment options for knee bone spurs.
What Is A Knee Spur?
Knee bone spurs, also called osteophytes, are small, hard lumps of excess bone that grow and project into the knee joint. They typically develop when there is excessive pressure on the knee bones from a lack of cartilage.
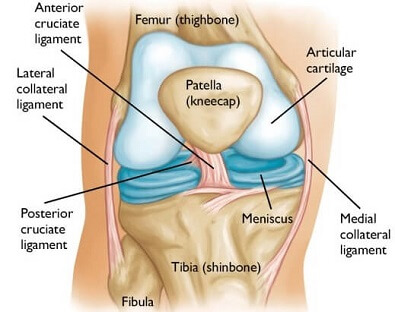
The knee joint is the meeting point between the thigh bone (femur) and the skin bone (tibia). It is a hinge joint that allows you to bend and straighten your leg.
In the middle of the “hinge” is a cushioning material called cartilage that covers the ends of the two bones.
There is also another extra thick layer of cartilage on top of the tibia, known as the meniscus.
The knee cartilage acts like a shock absorber and helps the bones to move smoothly against each other without any friction.
If the knee cartilage gets damaged or is put under too much pressure or friction, then the knee bones get irritated and inflamed as they rub against each other. The knee joint starts laying down new bone, a natural process known as osteogenesis, to try and protect itself and repair the damaged areas. If this goes into overdrive, it causes bone spurs in the knee to form.
How Do Knee Bone Spurs Form?
Knee bone spur formation goes through a few stages:
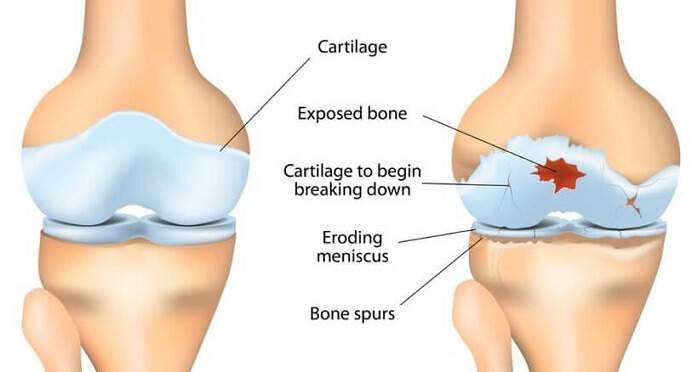
- Initial Joint Damage: The knee joint may experience various forms of stress or damage, such as repetitive motion, pressure, injury, or conditions like osteoarthritis. When this happens, the cartilage gradually degenerates, and the bony surfaces of the knee start to rub and place direct pressure against each other. This initial damage can cause changes in the joint structure and initiate an inflammatory response.
- Inflammatory Response: Inflammation occurs as a natural defence mechanism in the body for protection. When the knee cartilage is damaged, inflammation is triggered to promote healing. Inflammatory cells release certain chemical signals that stimulate the recruitment and activation of specialized cells called osteoblasts.
- Osteoblast Activation: Osteoblasts are bone-forming cells that play a crucial role in bone repair and remodelling. In response to the inflammatory signals from the cartilage damage, osteoblasts become activated and start depositing new bone tissue in the affected area of the knee joint.
- Excessive Bone Growth: As the osteoblasts deposit new bone tissue, it gradually extends along the edges of the existing bone, leading to the formation of bone spurs. These spurs are essentially excess bone that grows in response to the initial damage.
- Joint Changes and Implications: Over time, bone spurs in knee can cause changes in the joint's shape, structure, and function. They can impinge on nearby tissues, such as ligaments, tendons, or other bones, potentially leading to pain, restricted movement, and other symptoms.
Bone spurs in the knee usually grow slowly, forming over a few months or even years. The exact rate of growth can vary significantly among individuals, depending on factors such as the underlying cause, the extent of joint damage and the body’s response to the condition.
Bone growth with knee osteophytosis doesn’t tend to be steady or constant. This means the excess bone doesn’t usually grow at a uniform rate and the progression of knee spurs is often influenced by the underlying cause. There may be periods where the knee osteophytes develop rapidly, or in other cases their growth may slow down or stop altogether. Often, knee spurs reach a certain size and then remain relatively stable without significant further growth for an extended period, maybe even forever.
Common Knee Spur Causes
Bone spurs in the knee usually form in response to stress, pressure or damage to the knee joint cartilage and they are typically caused by:
1. Knee Arthritis
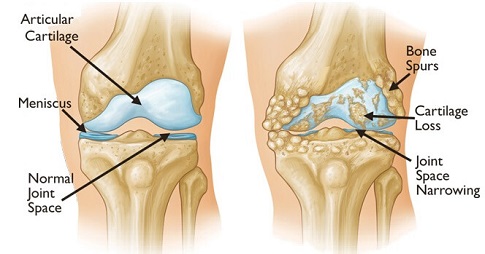
The most common cause of a bone spur on the knee is osteoarthritis, a type of degenerative joint disease.
Knee osteoarthritis causes wear and tear of the joint over time and the knee cartilage gradually breaks down. As the body tries to repair the damaged cartilage, it creates new bone material which over time builds up, forming knee spurs.
It is worth noting that while osteoarthritis is the most common cause of knee spurs, not all types of arthritis lead to bone spurs in the knee. For example, rheumatoid arthritis is an autoimmune condition where the body's immune system mistakenly attacks its own joints. This leads to joint damage and widespread inflammation throughout the body but isn’t as likely to cause bone spurs on the knee as osteoarthritis.
You can find out all about the causes, symptoms, diagnosis and treatment options in the Knee Arthritis section.
2. Previous Knee Injuries
If you have injured your knee in the past, you may be at increased risk of developing bone spurs in the knee in the future. Common knee injuries that increase the risk of knee osteophyte formation include:
- Meniscus Tears: damage to this thick layer of cartilage can leave parts of the knee joint surface unprotected. There may be tearing, fraying, thinning or complete loss of cartilage. Find Out More >
- Ligament Tear/Sprain: Overstretching or tearing one or more of the knee ligaments can result in instability. This instability can place excess friction or pressure through parts of the knee cartilage resulting in thinning and tearing of the cartilage. Find Out More >
- Fractures: a break in one or more of the knee bones or kneecap can disrupt the protective layer of cartilage covering the joint surfaces, triggering osteogenesis which can lead to knee spurs. Find Out More >
3. Age-Related Changes
Cartilage naturally deteriorates with age, becoming less elastic and less flexible. It loses water content making it less plump, and collagen fibres become less organised. This all causes the cartilage to become stiffer and more brittle, making it more prone to wear and tear and degeneration, increasing the risk of bone spurs forming in the knee.
4. Repetitive Stress
Certain occupations or activities that involve repetitive stress on the knee joint, such as kneeling, squatting, or running, can increase the likelihood of developing knee spurs. This is common in athletes, manual laborers and military personnel. The continuous pressure and strain on the knee can lead to the formation of bony outgrowths.
5. Repetitive Tension
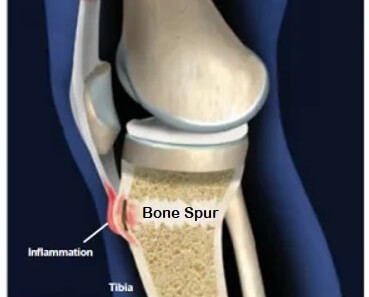
A bone spur under the knee is often caused by muscle tightness. The most common example of this is tightness in the quadriceps muscles.
The quads attach to the front of the shin bone at the tibial tuberosity, just below the knee, via the patellar tendon. If there is tightness in the quads muscles, it pulls on the tendon’s attachment point.
This creates a lot of tension on the bone, causing damage and inflammation, resulting in a condition called Osgood Schlatters Disease. Excess bone is laid down, resulting in a hard bump below the knee. Osgood Schlatters is the most common cause of a bone spur in the knee in teenagers, and often develops just after a growth spurt.
6. Other Causes
There are a few other things that can cause bone spurs in the knee to form such as
- Obesity: being overweight or obese puts extra pressure on your knees, particularly the inner side of the knee, putting you at increased risk of knee spurs
- Genetics: it is possible to have genetic predisposition to bone spurs on the knee. If your parents or grandparents have them, you are at greater risk of developing knee spurs
- Altered Foot Biomechanics: having flat feet changes the way the forces are directed through the leg, placing more pressure through the inner side of the knee. This increases the risk of medial knee spurs
- Diet: certain foods and drinks have be shown to increase the risk of knee spurs and osteoarthritis such as saturated and trans fats, highly processed food and refined carbohydrates. In contrast, certain foods can help reduce the risk such as oily fish and leafy green vegetables. Find Out More >
Bone Spurs In Knee Symptoms
In many cases, knee osteophytes are small and don’t actually cause any symptoms (asymptomatic) - people are often completely unaware they have bone spurs in their knees until they show up on an x-ray. But if the knee spur gets large enough that it starts encroaching on other structures, then it can cause problems.
Bone spur knee symptoms typically include:
- Knee Pain: bone spurs on the knee can cause pain, particularly if they start rubbing against other bones or soft tissues. There may be a sharp, catching pain as you move your knee or with weight-bearing activities, or more of a dull, background ache which is often worse after prolonged inactivity
- Knee Swelling: the inflammatory responses associated with bone spurs can lead to knee joint swelling. Knee spurs typically occur at the side of the knee so may cause localised side knee swelling, or there may be more generalised knee swelling involving a larger area around the knee joint
- Joint Stiffness: One of the most common bone spur in knee symptoms is knee stiffness. Bone spurs can limit the smooth movement of the knee joint and, if big enough, can actually partially or completely block movement in certain directions. Think of it like there being a wedge underneath a door. This stiffness can make it difficult to fully bend or straighten the knee and may be more pronounced after periods of inactivity. If bone spurs impede the normal range of motion in the knee joint it can cause limitations in activities such as walking, running, squatting and climbing stairs
- Clicking/Locking Sensations: Bone spurs in the knee can cause mechanical disruptions within the joint, resulting in knee popping or clicking sensations/noises during movement. If a bone spur on the knee breaks off, it can end up floating in the joint space and can cause knee locking, where the knee gets stuck and cannot move
- Weakness or Instability: Depending on the size and location of the knee bone spurs, they may affect the stability of the knee joint or interfere with the function of surrounding muscles and ligaments. This can lead to feelings of weakness or instability in the knee
- Numbness/Tingling: If the bone spur on the knee ends up compressing or irritating one of the nearby nerves, then you may experience pins and needles or reduced sensation around the knee, which may extend down the lower leg
- Bumpy/Knobbly Areas: you may be able to feel and/or see a hard lump on or around the knee. This most typically occurs at the edges of the knee joint or below the knee on the front of the shin.
Associated Problems
Knee bone spurs can increase the risk of developing other knee problems such as:
- Tendonitis: bone spurs can place excess friction through the surrounding knee tendons which can lead to inflammation and degeneration known as knee tendonitis. Common types of tendonitis linked with knee bone spurs include quadriceps tendonitis (above the knee), patellar tendonitis (just below the knee) and iliotibial band syndrome (outer knee)
- Bursitis: knee spurs may also place excess pressure on the knee bursa - small fluid-filled sacs that sit between soft tissues and bone. This can lead to pockets of swelling in various locations around the knee, depending on which bursa is affected. The most common types of knee bursitis linked with bone spurs are pes anserine bursitis (inner knee), infrapatellar bursitis (below the knee) and iliotibial bursitis (outer knee)
Diagnosing Bone Spur On Knee
The diagnosis of knee bone spurs is usually made by your doctor and typically involves a combination of taking a thorough medical history, a physical examination, and imaging studies.
- Medical History: Your doctor will begin by asking you about your knee symptoms, their onset, duration, and any factors that worsen or alleviate them. They will also ask about your medical history, previous knee injuries or surgeries, and any underlying conditions that may contribute to knee bone spur formation.
- Physical Examination: During the physical examination, they will assess your knee joint, looking for signs of inflammation, swelling, tenderness, and range of motion limitations that might indicate you have bone spurs in the knee. They may also perform specific manoeuvers or tests to evaluate the stability and integrity of the knee joint.
- Imaging Studies: If your doctor suspects bone spurs in the knee, they may send you for imaging tests to confirm the presence of knee spurs and assess their size, location, and impact on the knee joint such as:
X-Rays: X-rays provide detailed images of the bones and will highlight any bony abnormalities, including bone spurs
MRI (Magnetic Resonance Imaging): MRIs use magnetic fields and radio waves to generate highly detailed images of the soft tissues, including cartilage, ligaments, and tendons in and around the knee. MRIs can help evaluate the extent of joint damage, assess the condition of surrounding structures, and identify the presence of knee bone spurs. - Additional Tests: In some cases, additional tests such as ultrasound or CT scans may be used to provide further information about the knee joint and knee spur formation. These tests can help provide a more comprehensive evaluation and aid in treatment planning.
Early diagnosis of bone spurs in the knee is crucial for being able to effectively manage symptoms, prevent disease progression and minimise additional cartilage and joint damage.
Bone Spur Knee Treatment
Treatment for knee bone spurs aims to relieve symptoms, improve joint function, and address the underlying causes of the knee spurs. The specific treatment approach will vary depending on the severity of symptoms and individual circumstances.
Knee bone spurs treatment is only necessary if you are experiencing symptoms such as pain or restricted mobility.
#CommissionsEarned from Amazon on qualifying purchases
Non-Surgical Treatment
In many cases, bones spurs in the knee can be treated without the need for surgery, known as conservative treatment. Common bone spur knee treatment includes:
1. Pain Management
Over-the-counter painkillers, e.g. paracetamol/Acetaminophen and non-steroidal anti-inflammatory drugs (NSAIDs) e.g. ibuprofen/Advil can help reduce the pain and inflammation associated with knee bone spurs. Your doctor may prescribe stronger pain medications if necessary - always check with your doctor before starting any new medications.
2. Physical Therapy
Physical therapy is an important part of bone spur knee treatment and can help to not only relieve pain and improve range of motion, but can also slow down the progression of cartilage damage and knee spur growth.
Your physical therapist will devise a specific rehab program for you consisting of strengthening exercises and stretches to improve knee joint mobility, strength, and enhance overall joint stability.
They may also use other treatment modalities such as heat or cold therapy, electrotherapy, taping or joint mobilisations.
3. Knee Injections
Your doctor may advise trying knee injections as part of your knee bone spur treatment to reduce pain and inflammation. There are two options for knee injections:
Corticosteroid Injections: Injecting a mixture of anaesthetic and steroid directly into the knee joint can provide temporary relief from pain and inflammation. The effects may be felt for anything from a few days, to weeks or even months in some cases.
Hyaluronic Acid Injections: These injections, also known as visco-supplementation, involve injecting a gel-like substance into the knee joint to improve lubrication and reduce friction. Synvisc is a common brand used.
4. Assistive Devices
The use of assistive devices like knee braces, orthotics, or shoe inserts can really help alleviate pressure on the affected knee joint and provide support during activities to reduce pain from spurs on the knee and improve function
5. Lifestyle Modifications
Maintaining a healthy weight, adopting low-impact exercises e.g. cycling or swimming rather than running, and avoiding activities that exacerbate symptoms can help manage knee bone spur-related discomfort.
6. Arthritis Treatments
If your bone spurs in the knee are linked with osteoarthritis, there are a lot of other treatments that can help including acupuncture, natural remedies, walking aids, knee pads and rehab programs. You can find out all about them in the knee arthritis treatment section.
Bone Spur Knee Surgery
In some cases, bone spur knee surgery may be advised if you have failed to respond to non-surgical treatment or if the knee spurs are causing significant disability.
There are a two options when it comes to bone spur in knee surgery, depending on the extent of the joint damage:
1. Knee Arthroscopy
Arthroscopic knee bone spur removal surgery, aka keyhole or minimally invasive surgery, may be performed to remove or trim the bone spurs and smooth out damaged cartilage. A knee arthroscopy is the most common type of bone spur knee surgery performed and has good success rates.
2. Joint Replacement
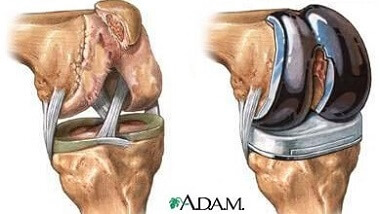
In severe cases where the joint damage is extensive, joint replacement surgery may be considered, with the damaged joint being replaced with an artificial joint.
Knee joint replacements are typically recommended for knee bones spurs associated with severe knee arthritis that has failed to respond to other treatment methods.
Depending on how much of the knee is damaged you may need one or both sides of the knee replacing. You can find out all about the different types of knee replacements, what happens and the recovery process in the knee replacement section.
The choice of bone spur knee treatment depends on factors such as the severity of symptoms, the impact on daily activities, overall health, and individual preferences.
Bone Spurs In Knee Summary
Knee bone spurs are a common problem, where excess bone grows, forming hard lumps, usually due to cartilage damage.
The most common cause of bone spurs in the knee is osteoarthritis, but they can also be caused by previous knee injuries, muscle weakness and tightness, aging, obesity and genetics.
In many cases, bone spurs on the knee do not cause any obvious symptoms and often go undetected.
Common bone spur in knee symptoms include knee pain, stiffness, joint restriction, knee popping, weakness, swelling and knee locking.
Bone spur knee treatment may involve a combination of medications, physical therapy, knee injections, orthotics, knee braces and in some cases bone spur knee surgery.
You may also be interested in the following articles:
- Front Knee Pain
- Swelling Below The Knee
- Kneecap Pain
- Burning Knee Pain
- Knee Pain At Night
- Knee Stiffness
- Knee Pain Diagnosis Chart
Page Last Updated: 06/02/24
Next Review Due: 06/02/26
Related Articles
Common Knee Problems
January 19, 2023
Knee Pain Diagnosis
January 10, 2023
Knee Strengthening
January 14, 2023
References
- Bone Spurs: What You Should Know About Osteophytosis - Healthline
- Association between patella spurs and quadriceps tendon ruptures - Muscles, Ligaments & Tendons Journal
- Osteophytes mediate the associations between cartilage morphology and changes in knee symptoms in patients with knee osteoarthritis - Arthritis Research & Therapy Journal